WHAT WAS CLAIMED
A graph showing Swiss COVID-19 mortality proves hydroxychloroquine is an effective treatment for the virus.
OUR VERDICT
False. The data used does not match official figures. Additionally, experts say the selective analysis of the data cannot be used to draw conclusions about the drug.
An Australian blogger has cited supposed changes in the fatality rate of COVID-19 sufferers in Switzerland as proof hydroxychloroquine is an effective treatment for the virus.
The claim is false. The data was originally published by a French website which has been accused of spreading misinformation.
The figures used do not align with official death counts from Switzerland. Regardless, biostatisticians said the analysis and interpretation of a small subset of Swiss data does not provide evidence hydroxychloroquine prevents COVID deaths.
The claim was made by Topher Field, a self-described commentator and libertarian who has previously made false claims based on misinterpretations of data (see here and here).
In a video originally posted to his Facebook page on August 22, 2020, Mr Field points to a graph that he says shows that the mortality rate of Swiss COVID cases dramatically increased between June 9 and June 26, 2020, after health authorities issued guidance warning health practitioners against using hydroxychloroquine to treat the virus.
According to the graph, Switzerland's COVID mortality rate then fell again after health authorities lifted hydroxychloroquine prescription restrictions on June 11.
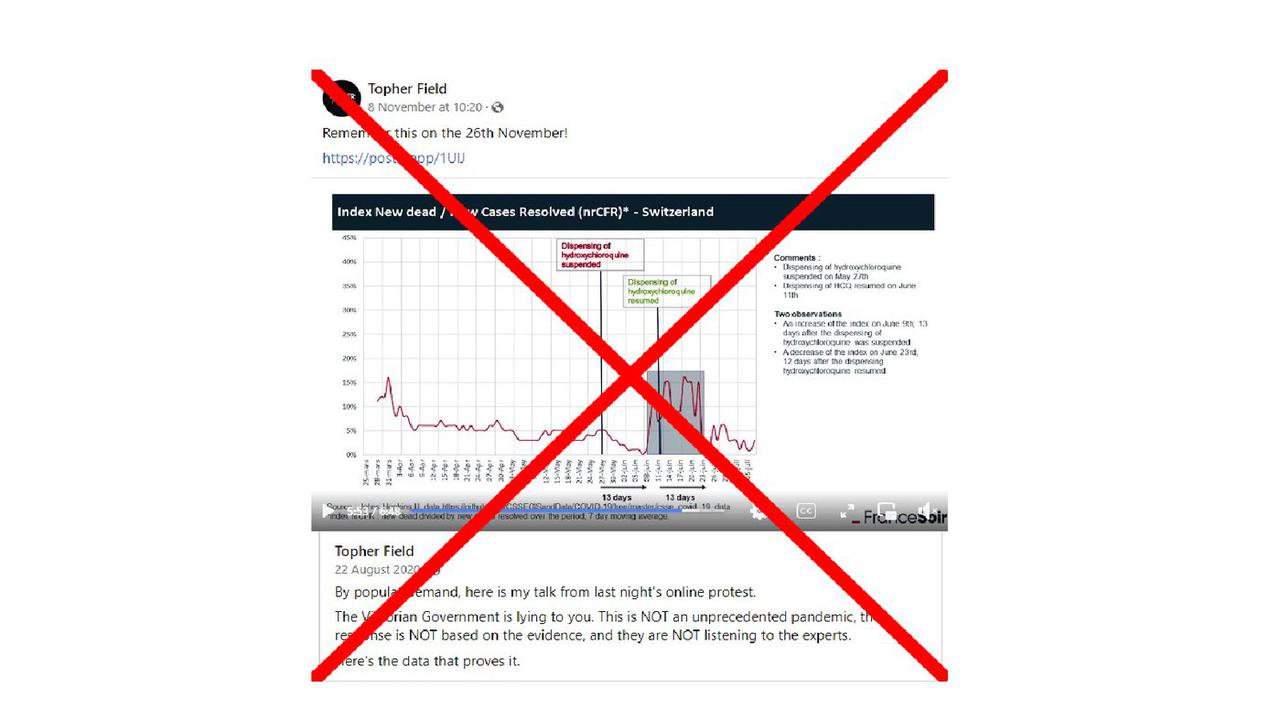
Mr Field republished on November 8, 2022, telling followers to remember the video on November 26 - the date of the Victorian election.
In the video he accuses the government of not listening to experts and not basing decisions on evidence.
"They would rather watch people die than allow them to get access to an effective treatment that would prove them wrong, " he says.
The graph, which was first published in July 2020 by French website FranceSoir, features a fatality measure called nrCFR.
Created by FranceSoir author Michel Jullian, the percentage figure comes from dividing the total number of deaths by the total number of cases over a seven-day period. Then multiplying by 100 to create a percentage.
The website applied a 13-day data delay to the changes in hydroxychloroquine guidance, which it suggested was the time it took for the changes to show up in the data. The reason for using a 13-day time lag is unclear.
Xavier Azalbert from FranceSoir, who was one of the authors of the article, did not respond to questions about why he had used a 13-day lag.
Hydroxychloroquine is an antimalarial drug promoted by Donald Trump in March 2020 as a treatment for COVID despite little evidence it worked.
Lab tests early in the pandemic provided some hope the drug could but later studies found it ineffective.
Health authorities in the US, Australia, the UK and elsewhere have recommended people do not use it to treat COVID.
The FranceSoir article draws its conclusions about the drug by analysing Swiss data taken from Johns Hopkins University.
However, the number of Swiss COVID deaths cited in the article does not match the data published by Johns Hopkins.
The FranceSoir article states that between June 9 and June 26, 2020, 35 people died with COVID in Switzerland.
Johns Hopkins only records nine COVID deaths.
Mr Azalbert also did not respond to questions about the source of his data.
Regardless of the accuracy of the data, biostatistics experts told AAP FactCheck they were not convinced by the statistical methods used in the article.
Associate Professor Paul Agius, a biostastistician at Deakin University and the Burnet Institute, said a significant limitation of the graph was that it was based on a small set of 'ecological' or population-level data (referred to in the article as "observational") which made it highly prone to spurious associations.
Mr Agius said a properly designed study such as a randomised controlled trial would be a more accurate way of measuring its efficacy or effectiveness.
"The article is incorrect to assert that their so-called observational data provides more compelling evidence than the results of numerous trials with respect to the treatment in question - randomised controlled trials are the gold standard here; by quite some margin," he said in an email.
"These ecological-level interrupted time-series type designs are typically only used where individual-level data are not available (or possible)."
He also said he did not recognise the nrCFR index used in the article.
Professor Annette Dobson, a biostatistics and epidemiology expert from the University of Queensland, similarly questioned the validity of the article's conclusions "on the grounds that there is lots of evidence that it (hydroxychloroquine) does not work".
"So either their result of a blip at that time was just a chance finding or there is some other explanation," she said in an email.
A third biostatistician, Associate Professor Shahid Ullah from Flinders University, said "the major problem" he saw was the uncertain latency period within the data, meaning the time it takes for cases to show up as positive and the time it takes for positive cases to result in death.
"Usually the case fatality ratio is the number of deaths detected among the observed cases/ total number of observed cases. But with COVID, it is not the deaths detected among the observed cases, it is the deaths that have been observed from the previous period, rather than the current period," Dr Ullah said in an email.
"If you want to establish causality between an intervention and a consequence, simple co-occurrence is not good enough. There has to be a plausible relationship between cause and effect."
Dr Ullah also questioned why the article based its conclusions on the time lag between the prescription changes and the alleged change in case fatality rates, saying it is unclear "why that would be exactly 13 days".
Switzerland's federal health department told AAP FactCheck that it asked FranceSoir to make corrections to the article "but our feedback was ignored".
"Based on our data, we did not see an increase in the number of deaths in Switzerland during the period mentioned in the article," a spokesman said in an email.
Brazil's Estadão Verifica has previously fact-checked a similar claim.
The Verdict
The claim that Swiss COVID data proves hydroxychloroquine is an effective treatment for the virus is false. The claim was based on data analysis by a French website but the figures do not match official Swiss COVID death numbers.
Regardless of the accuracy of the data, biostatisticians told AAP FactCheck the website's analysis and interpretation of a small sample of data was a poor way to assess the effectiveness of hydroxychloroquine. Multiple scientific studies have found it to be ineffective against COVID.
False - The claim is inaccurate.
AAP FactCheck is an accredited member of the International Fact-Checking Network. To keep up with our latest fact checks, follow us on Facebook, Twitter and Instagram.